In the pharmaceutical world, we often focus on the “Top Line”: India’s domestic market at $25 billion (₹2.12 lakh crore) and the global market approaching $2.6 trillion (₹221 lakh crore). But there is a second, more dangerous number that rarely appears on a profit and loss statement: $500 billion (₹42.5 lakh crore).
According to 2025–2026 analyses from Frontiers in Pharmacology and OECD health working papers, the global economic burden of medication non-adherence—the failure to take prescriptions as directed—exceeds $500 billion (₹42.5 lakh crore) annually. This is the “Global Adherence Leak”: money wasted not on buying drugs, but on the catastrophic medical complications that occur when patients skip them.
For India, a nation where Non-Communicable Diseases (NCDs) cause 60% of all deaths, this leak is more than a financial drain—it is a public health crisis waiting for an entrepreneurial solution.

The Math: How a $0.50 (₹42) Pill Becomes a $50,000 (₹42.5 Lakh) Bill
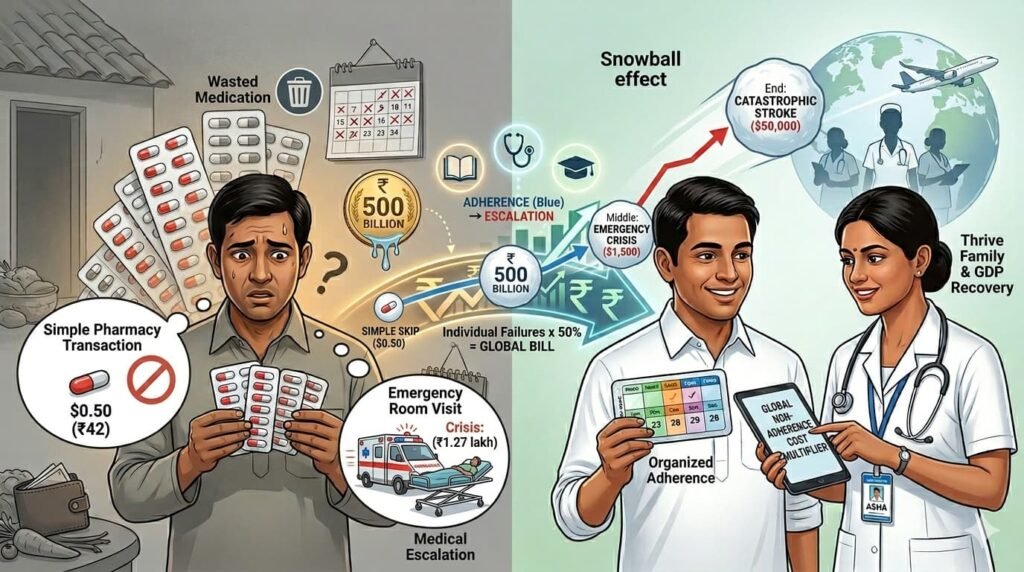
The economic burden of non-adherence follows a “snowball effect” that bridges the gap between a simple pharmacy transaction and a national economic crisis.
- Direct Costs: Wasted medication and unused prescriptions.
- Medical Escalation: A patient skips a $0.50 (₹42) blood pressure tablet. This leads to a hypertensive crisis, triggering an emergency room visit costing approximately $1,500 (₹1.27 lakh).
- Catastrophic Events: The crisis results in an ischemic stroke. The cost of surgery, ICU stay, and long-term rehabilitation can exceed $50,000 (₹42.5 lakh).
- Indirect Costs: The patient, often the primary breadwinner, loses months of productivity, impacting the family’s solvency and the nation’s GDP.
When you multiply these individual failures by the 50% of chronic patients globally who do not follow their regimen, the global bill surpasses $500 billion (₹42.5 lakh crore). In the United States alone, this leak is estimated at $100 billion to $300 billion (₹8.5 lakh crore to ₹25.5 lakh crore) annually.
The Indian Microcosm: Low Costs, Lower Adherence
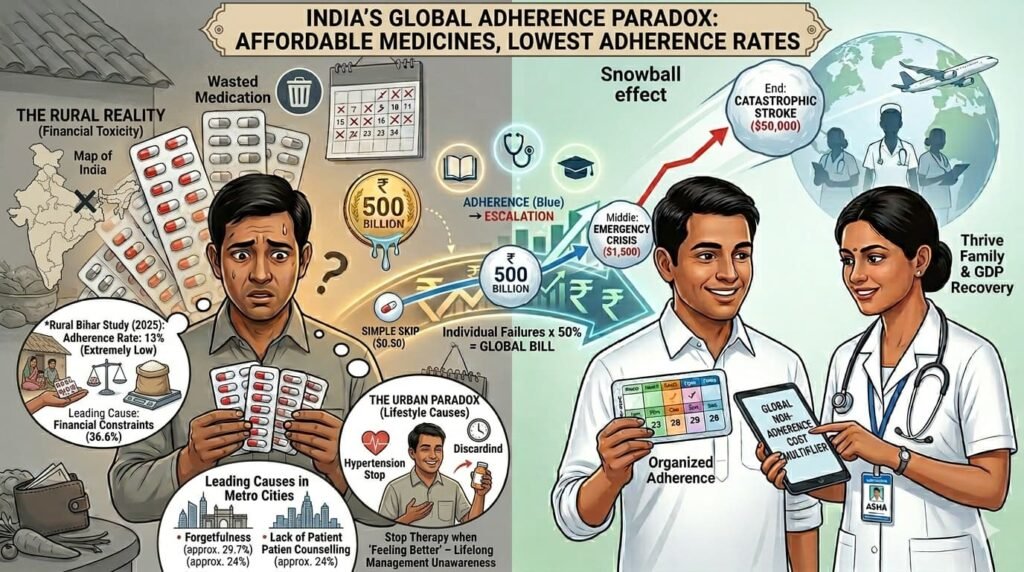
India presents a global paradox: some of the world’s most affordable medicines, yet some of the lowest adherence rates.
The Rural Reality
A 2025 study in rural Bihar found an adherence rate of only 13%. In these regions, the leak is driven by “financial toxicity.” Research shows that financial constraints are the leading cause of non-adherence in rural areas, accounting for 36.6% of cases. Even a “cheap” medicine is a luxury when it competes with the daily cost of food.
The Urban Paradox
In metro cities like Mumbai and Bengaluru, the leak is driven by lifestyle. Forgetfulness accounts for roughly 29.7% of non-adherence, while a lack of patient counselling is cited in 24% of cases. Here, patients often stop therapy the moment they “feel better,” unaware that silent killers like hypertension require lifelong management.
India’s Healthcare Workforce: The Untapped Trillion-Dollar Asset
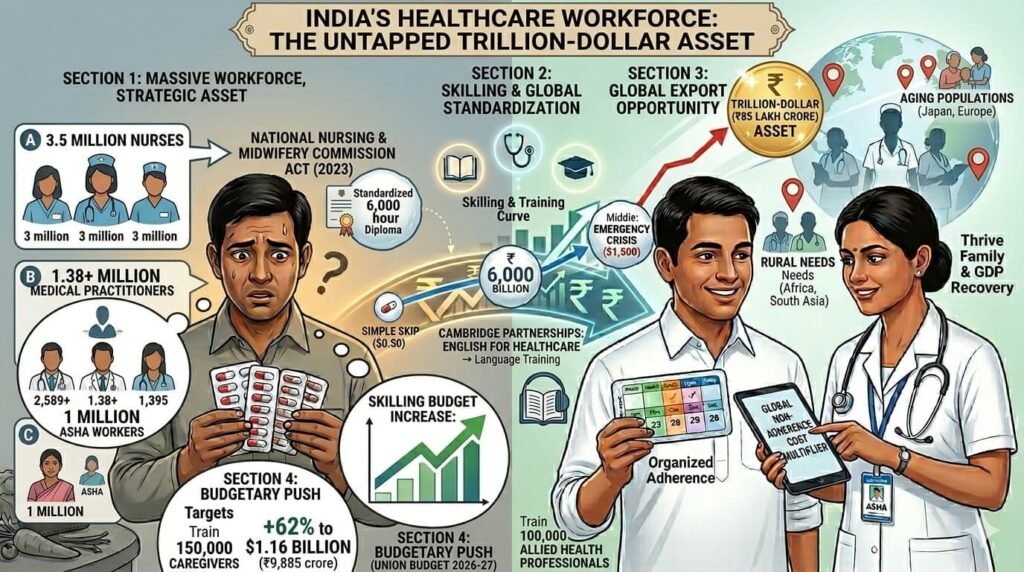
India currently possesses a massive workforce of 3.5 million nurses, over 1.38 million medical practitioners, and 1 million ASHA workers. Historically viewed as a domestic resource, this population is now a strategic export asset.
The Nursing Global Export
The global shortage of nurses stands at 4.5 million. With the National Nursing and Midwifery Commission Act of 2023 standardizing 6,000 hours of training, Indian nurses are being equipped for global mobility. Partnerships with institutions like Cambridge are training over 100,000 professionals in English for Healthcare to meet international standards.
The Budgetary Push
The Union Budget 2026-27 increased the skilling budget by 62% to $1.16 billion (₹9,885 crore). The goal is to train 150,000 caregivers and 100,000 Allied Health Professionals to serve both the aging populations of Japan and Europe and the expanding rural needs of Africa and South Asia. This is a potential trillion-dollar (₹85 lakh crore) services export opportunity hiding in plain sight.
Strategies for 2026: Closing the Gap
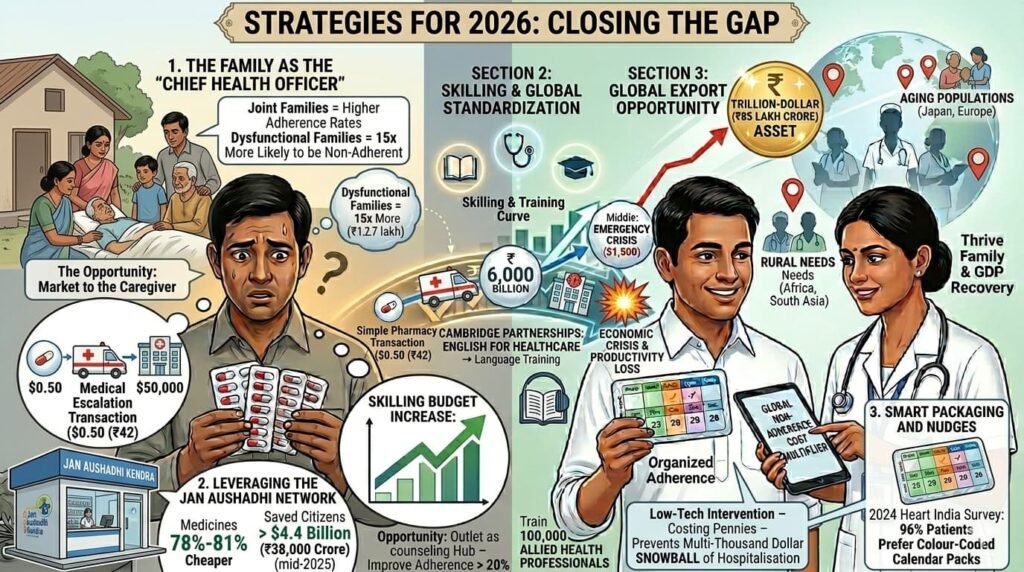
1. The Family as the “Chief Health Officer”
In India, patients in joint families have significantly higher adherence rates. Conversely, those in dysfunctional families are 15 times more likely to be non-adherent.
- The Opportunity: Marketing must target the caregiver. Educating a spouse or child is more effective than a digital reminder to a distracted patient.
2. Leveraging the Jan Aushadhi Network
With over 18,600 Kendras active in 2026, medicines are 78% to 81% cheaper than branded counterparts. This has saved Indian citizens over $4.4 billion (₹38,000 crore) as of mid-2025.
- The Opportunity: Transform these outlets into Counseling Hubs. A five-minute conversation at the point of sale can improve adherence by over 20%.
3. Smart Packaging and Nudges
A 2024 survey in Heart India found that 96% of patients prefer visually distinct, colour-coded “Calendar Packs.” This low-tech intervention—costing pennies—can prevent the multi-thousand-dollar “snowball” of hospitalisation.
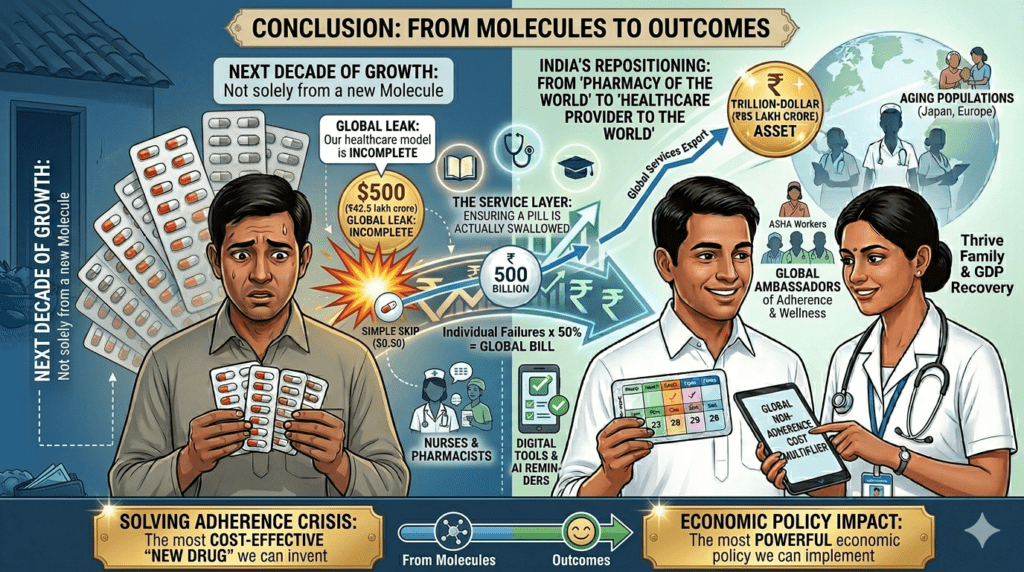
Conclusion: From Molecules to Outcomes
The $500 billion (₹42.5 lakh crore) global leak is a signal that our healthcare model is incomplete. For the Indian pharmaceutical industry, the next decade of growth will not come solely from a new molecule, but from the Service Layer—the nurses, pharmacists, and digital tools that ensure a pill is actually swallowed.
By repositioning its population—from ASHA workers to AYUSH doctors—as global ambassadors of “adherence and wellness,” India can move beyond being the “Pharmacy of the World” to becoming the “Healthcare Provider to the World.” Solving the adherence crisis is the most cost-effective “new drug” we can invent, and the most powerful economic policy we can implement.
Appendix: Sources and References
The following sources were utilized in the creation of this article. They include peer-reviewed journals, government data analyses, international health organization estimates, official government press releases, and industry reports.
Global Health Economics & Adherence Models
- Achterbosch, M., et al. (2025). Clinical and economic consequences of medication nonadherence: a review of systematic reviews. Frontiers in Pharmacology. (WHO data on 50% non-adherence and analysis of 43 reviews on mortality and resource utilization).
- OECD Health Working Papers (2025–2026 Update). Investing in Medication Adherence to Reduce Hospitalizations. (Methodology for the $500 billion [₹42.5 lakh crore] global extrapolation based on European cost data).
- IQVIA Institute Report (March 2026). Global Medicine Use 2026: Trends and Projections. (Verification of the $2.6 trillion [₹221 lakh crore] global pharmaceutical market).
- Iuga, A. O., & McGuire, M. J. (2014). Adherence and health care costs. Risk Management and Healthcare Policy. (The standard health economic model for the “snowball effect” from a missed dose to catastrophic costs).
- The Pharmacist (UK) (2025). Interview: Medication non-adherence at the root of drug pricing row. (Breakdown of intentional vs. unintentional adherence and remote monitoring solutions).
Indian Healthcare & Adherence Data
- Debbarma, S., et al. (2025). Medication adherence and its determinants among NCD patients in rural area of Bihar, India. Journal of Family Medicine and Primary Care. (Source for the 13% adherence rate in rural Bihar and the 15-fold risk increase in dysfunctional families).
- ScienceDirect (2025). EE55 Prescription Cost Dynamics in Chronic Disease Management: The Role of PMBJP-Scheme in Enhancing Affordability in India. (Source for the 78.11% average cost saving via Jan Aushadhi).
- Mahapatra, C., et al. (2024). Understanding the reasons behind medication nonadherence and exploring potential solutions. Heart India. (Metro vs. Non-metro breakdown: forgetfulness at 29.7% vs. financial constraints at 36.6%; 96% preference for color-coded packaging).
- Tolley, A., et al. (2023). Interventions to promote medication adherence for chronic diseases in India. Frontiers in Public Health. (Evidence for Community Health Workers and pharmacists as interventionists).
Government of India Policy & Workforce Reports
- Press Information Bureau (PIB) Delhi (2025). India-Australia Nursing Roundtable Concludes with Renewed Commitment to Global Collaboration. (Data on 157 new Government Nursing Colleges and the National Nursing and Midwifery Commission Act 2023).
- Economic Survey of India (2025–2026). Social Services Expenditure Surge. (Data on Out-of-Pocket Expenditure (OOPE) declining to 39.4% and savings of $14.7 billion [₹1.25 lakh crore] via Ayushman Bharat).
- Ministry of Ayush (2025). Initiatives towards integration of Ayush systems with Allopathic system. (Details on Dr. V.K. Paul’s advisory committee and AYUSH-ICMR Advanced Centres).
- Union Budget 2026–2027. Ministry of Skills Development and Entrepreneurship Allocation. (Data on the 62% increase in skilling budget to $1.16 billion [₹9,885 crore] for healthcare and allied training).
- AIIMS Rishikesh (2025). Official Inauguration of the Department of AYUSH and Integrative Medicine. (Documentation of the first fully functional integrative AIUSH department).
Industry & Regional Vision Documents
- Asianet Newsable (2025). Developed UP 2047: CM Yogi’s Vision. (Targets for a $6 trillion [₹510 lakh crore] state economy focused on health workforce density and medical tourism).
- Indian Television Dot Com (2025). Emversity and Cambridge Partnership. (Target to equip 100,000 nursing professionals with Cambridge English for Healthcare competencies by 2030).
Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. Pharmaceutical professionals should consult current regulatory guidelines and medical experts for specific patient care decisions.
Note: 2026 exchange rate approximation of $1 = ₹85.
The Hidden Crisis in Pharma: Why Face-to-Face Reps Are No Longer Enough
Why the future of pharma sales hinges on more than just pushing pills—it’s about understanding the evolving role of medical reps in a complex, high-stakes landscape.








